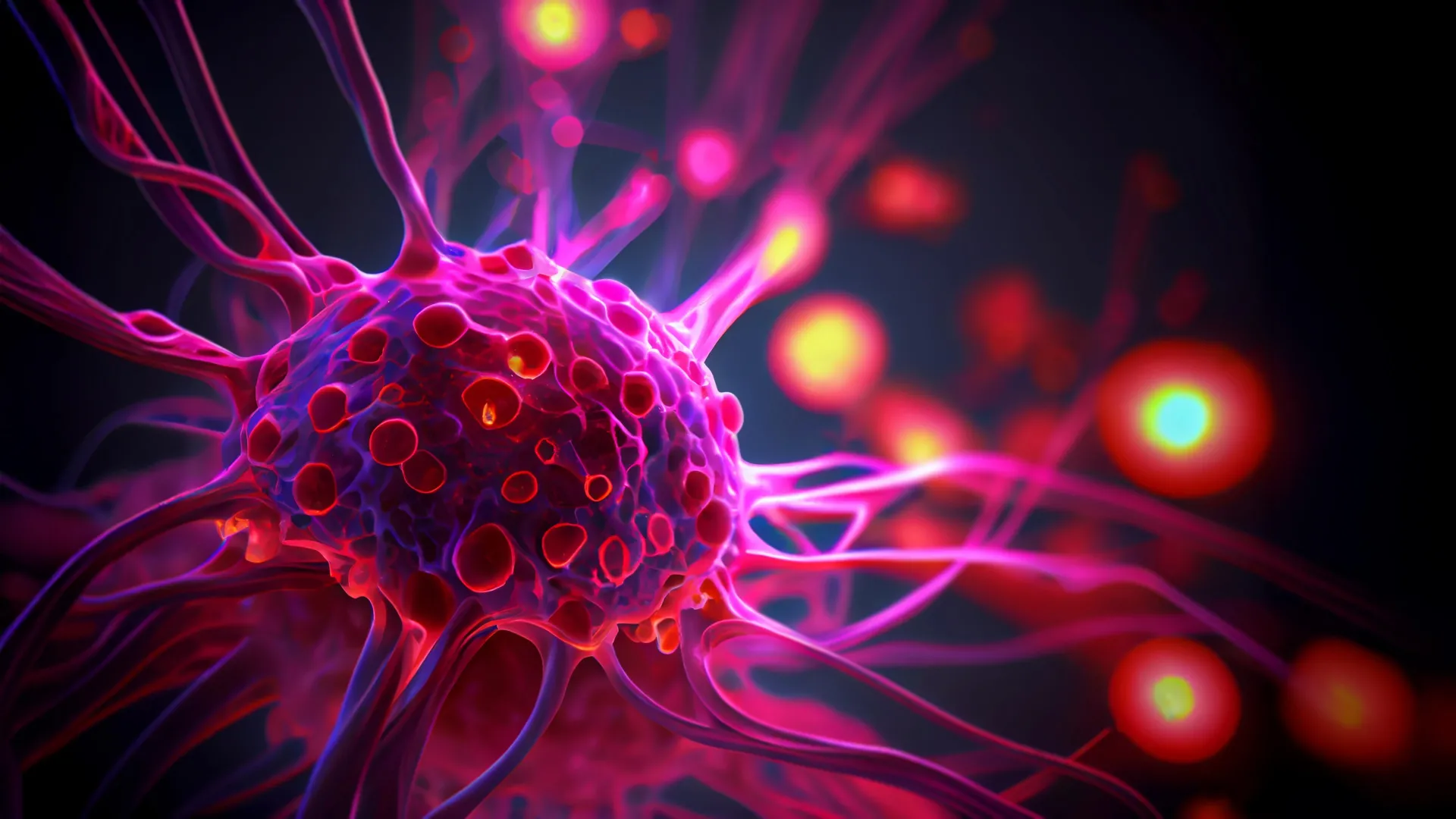
Researchers at the University of Geneva have discovered a significant mechanism by which tumors manipulate the immune system to promote their own growth. Their study reveals that neutrophils, typically known as the body’s frontline defense against infections, can be reprogrammed within tumors to instead support cancer development. This finding, published on February 10, 2026 in the journal Cancer Cell, highlights the complex interactions between cancer cells and the immune system.
Understanding how tumors grow and spread remains a critical challenge in cancer research. The collaborative work between the University of Geneva and the Ludwig Institute for Cancer Research sheds light on a surprising role neutrophils play in this process. These immune cells, when exposed to the tumor microenvironment, begin producing a chemokine known as CCL3, which actively encourages tumor progression rather than combating it.
Neutrophils: From Defenders to Tumor Allies
Neutrophils are among the most abundant immune cells in the human body and usually act as an early defense against infections and injuries. However, their presence in cancer cases often correlates with poorer outcomes. The research team found that tumors actively recruit neutrophils and alter their function. “We discovered that neutrophils recruited by the tumor undergo a reprogramming of their activity,” explains Mikaël Pittet, a professor in the Department of Pathology and Immunology at the University of Geneva. “They begin producing CCL3, which promotes tumor growth.”
This transformation illustrates how a protective immune response can shift to one that empowers cancer, complicating treatment strategies. The ability of these cells to adapt within the tumor environment underscores the importance of understanding cellular interactions in cancer progression.
Innovative Methods to Study Neutrophils
Studying neutrophils has proven challenging, particularly when it comes to genetic manipulation. “Neutrophils are particularly difficult to study and to manipulate genetically,” says Evangelia Bolli, co-lead author of the study and a postdoctoral researcher at the Broad Institute of MIT and Harvard. The research team employed various experimental strategies to precisely control the expression of the CCL3 gene in neutrophils without impacting other cell types.
By removing CCL3, researchers observed that neutrophils ceased to support tumor growth while maintaining normal function in the bloodstream. This finding emphasizes the potential for targeting specific pathways within immune cells to inhibit their tumor-promoting activities.
The team further validated their results by reanalyzing data from multiple independent studies. This analysis required the development of new techniques to accurately detect neutrophils, which often exhibit low genetic activity, making them difficult to identify using conventional methods. “We had to innovate to detect neutrophils more accurately,” notes Pratyaksha Wirapati, co-first author and bioinformatics specialist.
CCL3 as a Marker for Cancer Progression
The identification of CCL3 as a key driver of tumor growth offers a new avenue for understanding cancer evolution. “We are deciphering the ‘identity card’ of tumors by identifying the key variables that determine disease progression,” Pittet explains. This research suggests that a limited number of variables, once identified, could lead to improved patient management and more personalized treatment approaches.
The findings from the University of Geneva contribute significantly to cancer research by illuminating the dual role of neutrophils in the tumor environment. Understanding these mechanisms not only enhances the scientific community’s grasp of cancer biology but also paves the way for innovative therapeutic strategies aimed at mitigating the adverse effects of the immune system’s reprogramming within tumors.